When a newborn requires high-level care in an area that doesn’t have the capacity to support their needs, it’s critical that the infant’s healthcare team finds someone who does – and finds them fast. Throughout rural parts of the country, obstetric providers are often scarce, and hospitals don’t have the demand to maintain highly specialized neonatal teams for complex situations. North Memorial Health recently launched its air and ground NICU transport service for this exact reason, providing mobile neonatal intensive care transfers for babies born prematurely or with significant healthcare needs.
Immediate Neonatal Transfer – Day or Night
Available 24/7 in partnership with Minnesota Neonatal Physicians P.A., our transport team – which is led by a neonatal nurse and neonatal nurse practitioner, alongside our EMS crew, is ready to jump into action at any moment should the need arise.
“Every shift, we have three team members who are trained in providing NICU transport care, including a designated transport nurse,” says Noah Pardo, Manager of the Family Birth Center at Maple Grove Hospital. “With this model, when we receive a request for transfer, the team can immediately activate.”
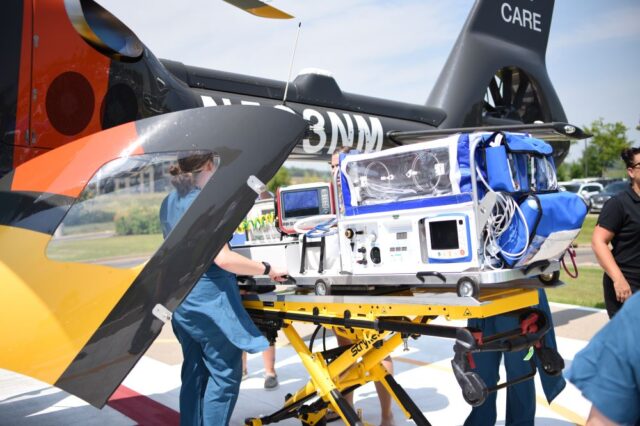
Our self-contained mobile neonatal intensive care units have capacity to stabilize patient temperature, deliver IV fluids and medications, and supply breathing support until the infant arrives at our NICU – providing acute support for complex patients during a critical time.
Ensuring Top-Notch Clinical Care and Safety
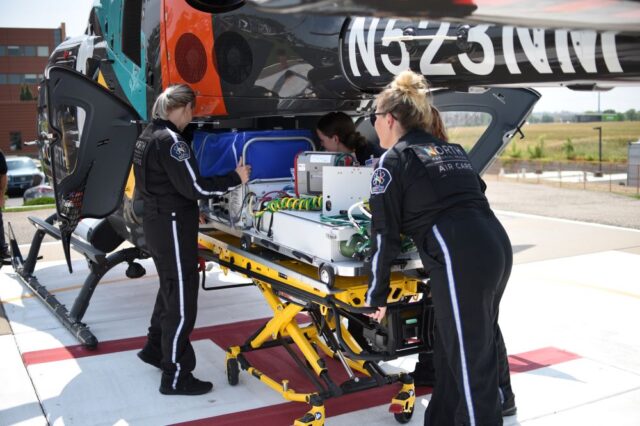 Building a highly experienced, extensively trained care team is imperative for transporting this fragile population – and the leadership at North Memorial Health Hospital and Maple Grove Hospital didn’t take this task lightly.
Building a highly experienced, extensively trained care team is imperative for transporting this fragile population – and the leadership at North Memorial Health Hospital and Maple Grove Hospital didn’t take this task lightly.
“All of the neonatal nurses hired onto the transport team went through a multi-step interview process to ensure they had expertise in Level III NICU care or NICU transportation,” said Pardo. “With that in mind, we already knew that we were bringing in an experienced clinical team.”
Training was conducted for skills that go beyond standard practice in the hospital setting, with all transport clinical team members attending flight training for in-air safety as well as in-services for the isolette setup and new equipment that will help provide care and transport the infant. All transport team members spent hours learning the new equipment and completed skills and equipment competencies for every aspect of care they will provide.
“Skills training was required for aspects of critical care that the neonatal nurses and nurse practitioners already do in the hospital but using new equipment and in a smaller, more confined space,” says Jessica Olson, NICU Nurse Clinician/Educator at Maple Grove Hospital. “They were all required to pass competencies on cares such as intubation, ventilation, securement of the endotracheal tube, suctioning, and administering surfactant to the baby’s lungs among other skills.”
Scenario simulation days were conducted routinely alongside EMS to run through the entire process, from receiving the referral and loading the isolette into the ambulance or helicopter to delivering cares while in transport – ensuring that when it is time to transfer a patient, everyone is fully prepared to put the steps in action and respond to the need as efficiently as possible. Air transfers will be done in our new Airbus H135 helicopter, which was recently added to our fleet due to its modern technology, with improved safety and advanced patient care outcomes as a result.
Support from Start to Finish
 From the moment the neonatology group receives a call for transport, our expert team provides comprehensive support for the referring hospital and parents of the newborn through each step in the process, from activation to post-transport updates. These support systems are put in place to help everyone feel confident and comfortable in the transport process as we all work together to deliver the highest level of care for the neonatal population.
From the moment the neonatology group receives a call for transport, our expert team provides comprehensive support for the referring hospital and parents of the newborn through each step in the process, from activation to post-transport updates. These support systems are put in place to help everyone feel confident and comfortable in the transport process as we all work together to deliver the highest level of care for the neonatal population.
“When the NICU team gets to the patient at the referring facility, they’ll ensure the newborn is stabilized and then they call the neonatologist to update them on patient status, what has been done care wise, and confirm any additional treatments or cares that should be done immediately,” says Billie Sell, Air Care Clinical Manager. “With this process in place, the team will have the most up-to-date orders from the provider and can start needed treatments immediately in transport.”
Recognizing the anxiety and concern that comes with parents preparing to have their baby transported, our team is also dedicated to keeping them as informed and up to date as possible, providing detailed updates and a packet with information on when and exactly where their baby will arrive to our hospital, a number they can call at any time for support, and any other details for what to expect in the transfer.
Transport Prior to Delivery
The safest option for complex pregnancies is to transport high-risk mothers prior to delivery to a hospital where teams are prepared to handle complicated deliveries and fragile newborns. At North Memorial Health Hospital and Maple Grove Hospital, expectant mothers have access to maternal fetal medicine specialists, level II-III NICUs and OB hospitalists to provide care and support in their journeys.
When transport prior to delivery isn’t an option, mobile neonatal intensive care units are just a phone call away.
Indicators for Neonatal Transport
While there are a number of reasons a newborn could require transport to another hospital for more intensive care, some of the most common reasons include:
- <34 weeks or <1500 grams
- Respiratory distress needing >40% FiO2
- Need for assisted ventilation
- Suspected heart disease
- Suspected infection
- Metabolic disorders including hypoglycemia
- Congenital anomalies
- Seizures
